
Hospital Onset Bacteremia (HOB): Let’s Talk About Reporting
For several years there has been a lot of chatter about potential future expansion of bloodstream infection surveillance to move beyond only Central Line-Associated Bloodstream infections (CLABSI) and expand to include all hospital onset bacteremia (HOB). As this gets closer to being a reality for programs, it is important to understand what this does and does not mean. As of the June 2023 Healthcare Infection Control Practices Advisory Committee (HICPAC) meeting and the national APIC conference, the Centers for Disease Control and Prevention (CDC) has indicated that the module for HOB is anticipated to be available to hospitals some time in 2024. They have already been piloting the protocol with some facilities since earlier this year. This will be voluntary reporting at this time for all inpatient facilities currently enrolled in National Healthcare Safety Network (NHSN), not including longterm care or outpatient dialysis. Centers for Medicare and Medicaid Services (CMS) put out a call for comments last year about potential future adoption of HOB as one of their measures, but no timeline has been given on when that may put into place. Currently, the measure is working its way through the endorsement process; with the transition from National Quality Foundation (NQF) to Batelle midway through the cycle making that timeline a little less clear. It is anticipated that the endorsement vote will occur at the August 2023 meeting.
What Exactly is HOB & Why is this Surveillance Expansion Being Considered?
HOB is a much broader metric than the current central line only surveillance that most organizations perform for bloodstream infections. It recognizes that there are risks beyond just central lines and beyond just vascular access devices. Recent studies confirm that the impact of these infections in terms of costs, length of stay and in hospital mortality are similar to those associated with CLABSI yet the case burden is four times higher.1 The protocol is intended to be fully automated, which will drastically reduce the surveillance burden on infection prevention teams. NHSN Digital Quality Measures (dQMs) are “fully-automated, digital quality measures based on standards, measurement science, and clinical science that are used to drive patient-safety with rigorous benchmarking and appropriate risk-adjustment.”

Using Fast Healthcare Interoperability Resources (FHIR), information will be collected on all positive blood cultures with pathogenic bacteria or fungi from Emergency Departments, observation patients, and inpatients. Manual reporting or CDA transmission will not be an option for this surveillance module. Those positive specimens collected on or after hospital day four will be classified as hospital onset. In addition to the primary HOB metric, there are complementary measures which will be used for risk adjustment and internal quality improvement efforts including blood culture utilization, blood culture contamination, community-onset bacteremia & fungemia, matching commensal HOB. Until the protocols are finalized and implemented in the portal there is the possibility that some changes may be introduced, but the above framework is what has been shared by CDC to this point.2
HOB: What is it NOT
It is important to realize that HOB is different from peripheral IV bloodstream infection reporting, which many of us had been hoping for, but it is a great starting point for infection prevention and vascular access and infusion specialty teams to partner to review contributing factors for cases identified in the organization. Because all HOB will be reported, regardless of source of the infection, it makes sense that a collaborative review take place to identify potential contributing factors whether they are device-related, procedure-related or otherwise. Teams can review the cases and indwelling devices to understand where their organization’s biggest remaining opportunities for reducing preventable HOB.3
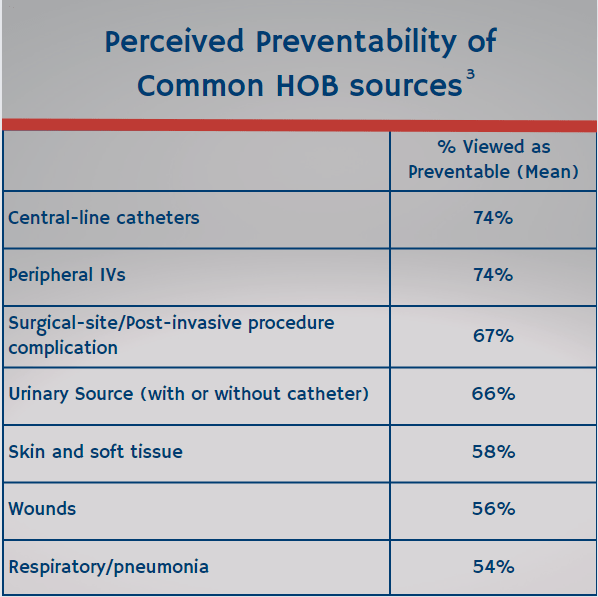
Why Wait for CMS Quality Measure Mandate?
Peripheral IVs and midline catheters are likely included in those risks, based on what has been seen in the literature over the past decade. Understanding the insertion, care and maintenance of those devices and the related risk reduction strategies can positively impact patients, as well as (eventually) what will likely become public reported and incentivized measures. Developing those relationships within your facility now can help create a framework for consistently reviewing cases in a collaborative manner and then developing interventions to address the identified contributing factors. Using what we have learned over the years with CLABSI prevention, optimizing insertion is a necessary first step but equally important is ensuring that devices are properly cared for and promptly removed when no longer necessary.
Reach out to your industry partners, such as Eloquest Healthcare, who can assist you with bedside audits of current opportunities and provide education and solutions to help address potential areas for risk reduction to your patients far beyond just central lines.
Eloquest Healthcare is committed to providing solutions that can both improve patient outcomes and reduce unnecessary costs. We work with your institution to perform a bedside audit evaluating vascular access device sites to assess infection risk and quality improvement. Click here to request a Vascular Access Device Site Audit today!

References:
- Yu, K et al. Characteristics, costs, and outcomes associated with central line- associated bloodstream infection and hospital-onset bacteremia and fungemia in US hospitals. ICHE, in press
- Centers for Medicare and Medicaid. List of measures under consideration for December, 2021. Accessed July 13, 2023. https://www.cms.gov/files/document/measures-under-consideration-list-2021-report.pdf
- American Hospital Association. HOSPITAL ONSET BACTEREMIA Hospital leaders’ attitudes on HOB sources, prevention and treatment. Accessed July 13, 2023. https://www.aha.org/system/files/media/file/2023/04/BD_HospitalBacteremia_ebook_040523.pdf







