Use the table below to browse our clinical evidence or sort by keyword. To access the data click the ‘View’ column.
Mastisol Clinical Evidence & Resources
Sales Materials & Resources
Clinical Evidence
| wdt_ID | Category | Author | Key Findings | Purpose | Setting | What was being adhered? | View Data |
|---|---|---|---|---|---|---|---|
| 1 | Adherence | Mikhail et al.¹ | Mastisol was found to be significantly better than TOB in increasing adhesiveness. | Compared Mastisol and tincture of benzoin (TOB) for their abilities to increase the adhesive power of wound closure strips. | Artificial clinical setting/volunteers | Wound closure strips | View |
| 2 | Adherence | Moy et al.² | Mastisol significantly increased the adhesiveness of all wound closure tapes tested. | Evaluated adhesive properties of 7 different wound closure tapes with and without Mastisol. | Artificial clinical setting/volunteers | Wound closure tapes | View |
| 3 | Adherence | Patient Safety | Lesesne³ | After 5 days, 60 (40%) patients in the TOB-treated group vs 10 (7%) in the Mastisol-treated group showed signs of loss of adhesiveness. Temporary contact dermatitis developed in 38% of the TOB-treated patients vs 0.7% of the Mastisol-treated patients. Four patients in the TOB-treated group developed superficial skin infections vs none in the Mastisol group. | Compared Mastisol and TOB for adhesive properties and potential complications in a study of 300 patients with woundclosure strips. | Surgical suite | Wound closure strips | View |
| 4 | Adherence | Katz et al.⁴ | Failure to coat the entire skin surface with Mastisol was detrimental to strip adherence. | Investigated the optimal pattern of surgical strips needed to maximize adhesiveness. | Artificial clinical setting/volunteers | Wound closure strips | View |
| 5 | Adherence | Patient Safety | Yavuzer et al.⁵ | Mastisol significantly increased the adherence of adhesive strips. Mastisol significantly improved the burst strength of wounds closed with adhesive strips alone. | Compared burst strength of skin closure with sutures alone vs sutures with adhesive strips, with and without Mastisol. | Artificial laboratory setting/cadavers | Wound closure strips | View |
| 6 | Adherence | Patel et al.⁶ | Pretreatment of the skin with Mastisol significantly increased the pullout force needed to dislodge the catheter for all tapes studied, either alone or with TOB pretreatment. | Investigated “pullout force” needed to dislodge IV catheter secured with various tapes, both alone and with the addition of TOB or Mastisol. | Artificial clinical setting/volunteers | Tapes attached to IV catheter | View |
| 7 | Patient Safety | James et al.⁷ | 16/~4500 cadets (0.3%) treated with TOB developed contact dermatitis severe enough to render them unfit for duty. 0/2200 (0%) cadets treated with Mastisol over 2 years developed contact dermatitis. | Evaluated West Point military cadets during basic training for allergic contact dermatitis following treatment for friction blisters with TOB or Mastisol. | Military clinical setting | N/A | View |
| 8 | Patient Safety | Klein et al.⁸ | Clinician unable to work for 10 days while dermatitis was treated. | Described severe contact allergic dermatitis in anesthesiologist exposed to tincture of benzoin. | Operating room | Small bandage with TOB | View |
| 9 | Patient Safety | Ryder and Duley⁹ | No significant difference in the reduction of normal skin flora was observed on skin prepped with CHG/IPA vs skin prepped with CHG/IPA followed by Mastisol or Detachol. Use of Mastisol or Detachol did not affect the antiseptic effectiveness CHG/IPA. | Evaluated compatibility of 2% clorhexidine gluconate/70% isopropyl alcohol (CHG/IPA) with Mastisol and Detachol to determine whether either product affected the antiseptic effectiveness of CHG/IPA. | Laboratory setting/ volunteers | N/A | View |
| 10 | Adherence | Patient Safety | Deneau and Craig¹⁰ Cookeville Regional Medical Center |
With Mastisol use, fewer dressings were compromised prior to 7 days. | Nursing staff noted less damage to patients’ skin while productivity was maintained. | Evaluated effectiveness of Mastisol for enhancing CVC dressing securement and preventing detachment. | ICU | CVC dressings | View |
| Category | Author | Key Findings | Purpose | Setting | What was being adhered? | View Data |
Need more assistance? We’re happy to connect you with your local representative, give us an email at information@eloquesthealthcare.com!
Mastisol Video Library
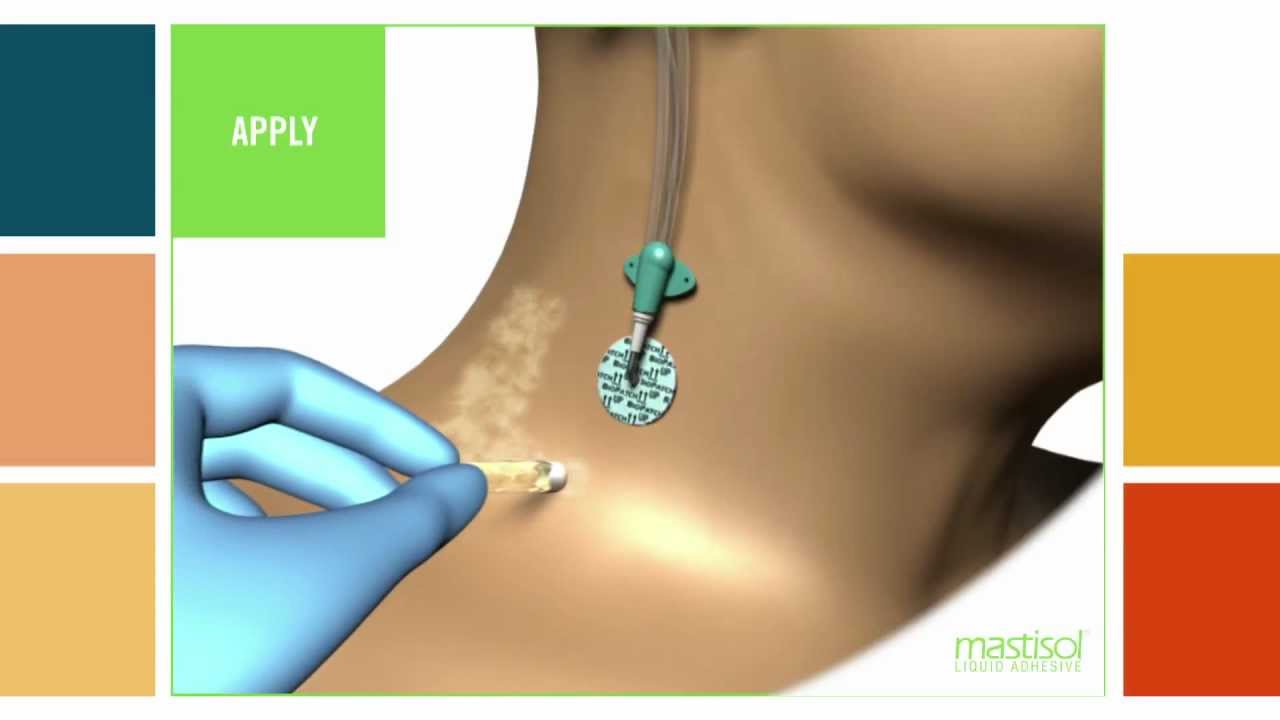
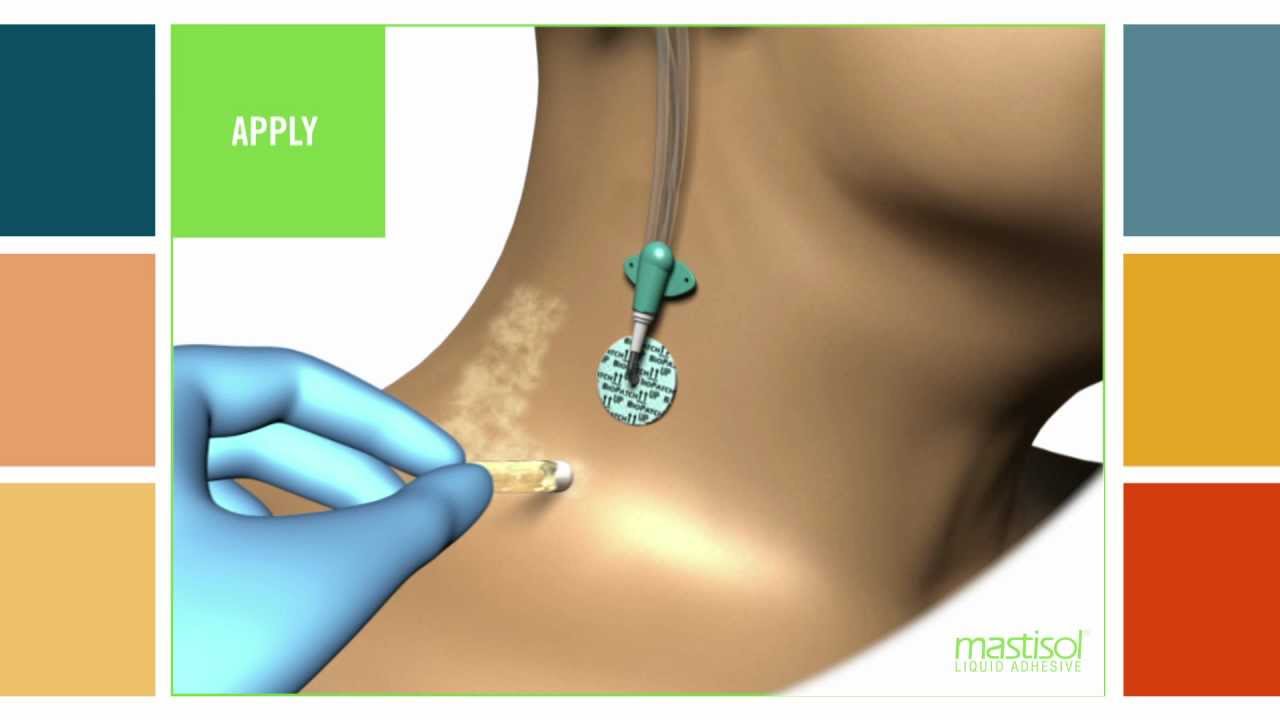







References
- Mikhail GR, Selak L, Salo S. Reinforcement of surgical adhesive strips. J Dermatol Surg Oncol. 1986;12: 904-6.
- Moy RL, Quan MB. An evaluation of wound closure tapes. J Dermatol Surg Oncol. 1990;16:721-3.
- Lesesne CB. The postoperative use of wound adhesives. J Dermatol Surg Oncol. 1992;18:990.
- Katz KH, Desciak EB, Maloney ME. The optimal application of surgical adhesive tape strips. Dermatol Surg. 1999;25:686-8.
- Yavuzer R, Kelly C, Durrani N, Mittal V, Jackson IT, Remine S. Reinforcement of subcuticular continuous suture closure with surgical adhesive strips and gum mastic: is there any additional strength provided? Am J Surg. 2005;189:315-8.
- Patel N, Smith CE, Pinchak AC, Hancock DE. The influence of tape type and of skin preparation on the force required to dislodge angiocatheters. Can J Anaesth. 1994;41:738-41.
- James WD, White SW, Yanklowitz B. Allergic contact dermatitis to compound tincture of benzoin. J Am Acad Derm. 1984;11:847-50.
- Klein TG, Woehlck HJ, Pagel PS. Severe allergic contact dermatitis resulting from occupational exposure to tincture of benzoin aerosol spray in an anesthesiologist. J Anesth. 2009;23:292-4.
- Ryder M, Duley C. Evaluation of compatibility of a gum mastic liquid adhesive and liquid adhesive remover with an alcoholic chlorhexidine gluconate skin preparation. J Infusion Nursing. 2017;40:245-52.
- Deneau J, Craig A. Nursing survey reveals novel strategy in assisting adherence to best practices of CVC dressing management. Presented at: Institute for Healthcare Improvement National Forum; December 8-11, 2013; Orlando, FL.
- Pullen D. Quality Improvement Initiative to Improve Dressing Adherence Reveals Improved Dressing Adherence Observations on a Before-After Analysis. Presented at: Association for Vascular Access Annual Scientific Meeting, September 7-10, 2014; Washington DC.
- Niehaus S, McCord J. Improving Adhesion of Internal Jugular Dressings in the Intensive Care Unit. Presented at: Association for Vascular Access Annual Scientific Meeting, September 16-19, 2016;Orlando, FL.
- Browne B, Moffo H. Quality Improvement Initiative Results in Fewer Dressing Disruptions and Improved Adherence to Best Practices. Presented at: Greater Cincinnati AACN Chapter, 28th Annual Trends in Critical Care Conference, April 8, 2016; Cincinnati, OH.
- Bortz A, Hardinger K, Peltzer J. Impact of implementing Mastisol in central line dressing changes on central line-associated blood stream infections in progressive care units: a quality improvement project. Presented at: Magnetizing KC Symposium, February 24, 2015.
- Aldi R, Galvin K, Weintraub S, et al. Quality improvement initiative results in the standardization of processes for central line-associated bloodstream infection prevention and increased adherence to best practices. Presented at: AACN Horizons Conference, October 8-9, 2018; Manchester, NH.
- Jameson L. From PRN to routine…a vascular access team’s journey to reducing PRN central venous catheter dressing changes by adding to the vascular access tool box. Presented at: Association for Vascular Access Annual Scientific Meeting, September 15-18, 2018; Columbus, OH.
- Squires EN, Bruggeman S. Use of gum mastic medical adhesive to maintain central venous access device dressing integrity. Presented at: Association for Vascular Access Scientific Meeting, October 4-7, 2019; Las Vegas, NV.
- Boudreaux A. Ventriculostomy Dressing Process Improvement. Presented at the National Teaching Institute & Critical Care Exposition, May, 2013; Boston, MA.
- DeVries, M; Sarbenoff, J; Scott, N; Wickert, M; Hayes, L. Improving Vascular Access Dressing Integrity in the Acute Care Setting, Journal of Wound, Ostomy and Continence Nursing: June 28, 2021 – Volume Publish Ahead of Print – Issue – doi: 10.1097/WON.0000000000000787
- Vowels S. Quality Improvement Project to Assess the Impact of Gum Mastic Liquid Adhesive on the Integrity and Durability of Driveline Dressings, Risk of Infection, and Patient Satisfaction. Journal of the Association for Vascular Access. 2023; 28(3): 31–37. doi: https://doi.org/10.2309/JAVA-D-23-00006
- Gamble JJ, McKay WP, Peeling A, Durr C, Krysak T, Guo R, Lange T, Cowen J, Bajwa JS. A comparison of methods used to secure pediatric endotracheal tubes using a live human dermal model. Can J Anaesth. 2021;68:645-52.

