Vascular Access is the most prevalent invasive medical procedure. While serious consequences can occur with this common procedure, ensuring optimal outcomes is possible.
Matthew Gibson, RN, CRNI, VA-BC, CPUI recently presented a three-part Wednesday Workshop series, “Stop Struggling with Vascular Access Device Outcomes”. It is Matt’s mission to improve vascular access and infusion practices and to eliminate associated complications. Matt has served on national and regional vascular access and infection control committees, written evidence-based education programs and speaks publicly on a range of vascular access and infusions techniques and practices. Matt brings this blend of skills and experience to the Wednesday Workshop series where this complex topic was broken into the following three quick presentations with actionable tips and resources:
Ideal Insertion
Superior Securement
Mastering Maintenance
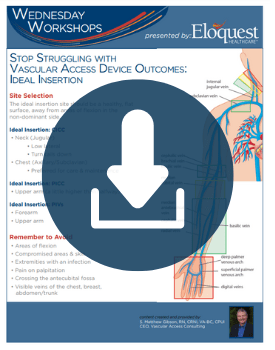
Ideal Insertion
Proper device, site, and vein selection leads to successful vascular access for the duration of therapy. The Zone Insertion Method, initially for PICCs, has been applied to all device types. General guidance for the ideal insertion site is a healthy, flat, surface, away from areas of flexion on the non-dominant site to promote self-care.
Ideal veins are straight, compressible, have smooth vein walls and contain no echogenic material. Veins that best accommodate the catheter should be 3X larger than the catheter. DOWNLOAD the Ideal Insertion Resource shared in this informational session.
Download Ideal Insertion Resource
Superior Securement
Device dislodgements are unacceptably high. Device-related bloodstream infections are a preventable complication. If you are not sufficiently paying attention to securement and stabilization at the site and the dressing, the device is not sufficiently protected.
Best practice guidelines recommend that all vascular access devices (VADs) be secured to prevent complications and improve outcomes. There is a variety of catheter securement methods, each with differing advantages. Securement can be transdermal, cutaneous, and subcutaneous.
Also, dressing securement guidelines recommend that the dressings be changed immediately if the integrity is disrupted. Guidelines also define a lifted dressing in need of attention as, “lifted/detached on on any border edge or within transparent portion of dressing.” Evaluate a combination of securement measures to reduce complications and device failure.
Download Six Steps to Superior Securement
Mastering Maintenance
The goal of VAD care and maintenance is to reduce the risk of complications and preserve the device function for the duration of therapy.
Common challenges that can occur in maintaining the device are:
- Dressing disruption
- Device migration/dislodgement
- Micropistoning of the device
- Compliance to aseptic technique
Download Mastering Maintenance Checklist
If you believe such a challenge is occurring at your facility, quality improvement is possible! Start by picking a framework for your quality improvement process. A resource for this process is available for DOWNLOAD using the Plan-do-Study-Act model.
If you need support, ask for help! Many vendor partners have programs that can assist with this process. Eloquest Healthcare, Inc. can partner with your institution to facilitate a Vascular Access Device Site Assessment to determine the state of both dressing and skin integrity for patients in your facility, while providing you and your team with information on your facility’s infection risk, nurse efficiency, and product waste. Click HERE to request a Point Prevalence Assessment today!