
Edward Korycka, RN has spent 20 of his 30 years in nursing specializing in vascular access. He is an active member of the Association for Vascular Access and Infusion Nurse Society, having served in various leadership positions. In his current role at Access Vascular, Korycka strives to improve patient outcomes by promoting training and support for the company’s novel vascular access device offerings. Korycka recently gave a webinar “Pathway to Patency: Exploring the challenges to catheter patency and the technology to help reduce them”. We’ve summarized the content below, and the webinar can be accessed here.
What is Catheter Patency?
Before delving into relevant practices, it is important to review the definition of catheter patency. While patency in general can be defined as the degree of openness of a tube with a relative absence of blockage, catheter patency is more detailed. Patency is an important part of both increasing catheter functionality and avoiding potential complications.

The Path to Catheter-Related Thrombosis (CRT)
Clotting is a protective response that is designed to prevent loss of blood due to bodily injury— however, the puncture of a catheter insertion into a blood vessel is sufficient to trigger the coagulation cascade. Thrombosis is a complication that is responsible for many catheter occlusions. While clotting in normal hemostasis conditions is a positive thing, inappropriate clotting responses can negatively impact patient outcomes.
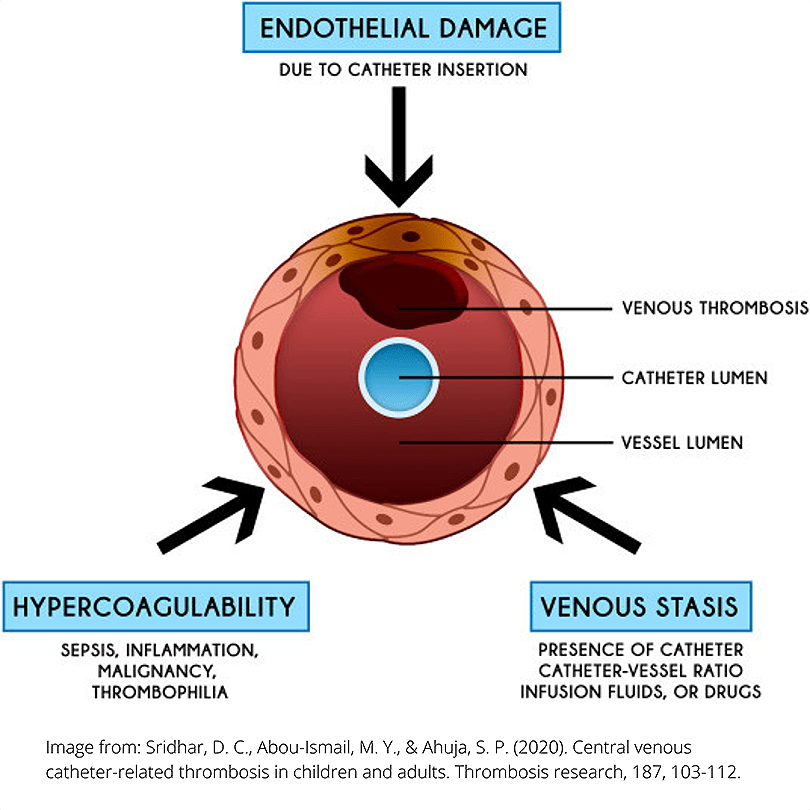
Thrombosis in deep veins of the arms and chest (subclavian, axillary, brachial) can lead to pulmonary embolism and sustained health issues even with prompt treatment. This issue is prevalent in in vascular access care, with intravenous catheters being responsible for 70-80% of thrombotic events that occur in the superficial and deep veins of upper extremities. Note that the introduction of a needle or catheter at any time can lead to thrombus formation. A triad of issues related to catheter use can increase the risk of thrombotic events: endothelial damage, hypercoagulability, and venous stasis.
Hypercoagulability conditions that must be considered when assessing your patient’s risk for thrombotic events include:
– Prolonged bed rest or immobility
– Obesity
– Central venous catheter placement
– Recent trauma or surgery
– Cancer
– Pregnancy
– Medications used to treat cancer, such as tamoxifen, bevacizumab, thalidomide and lenalidomide
– Supplemental estrogen use, including oral contraceptive pills (birth control pills)
– Previous history of deep vein thrombosis or pulmonary embolism
– Inflammatory bowel syndrome
– HIV/AIDS
The four types of potential catheter-related thrombus (CRT) are:
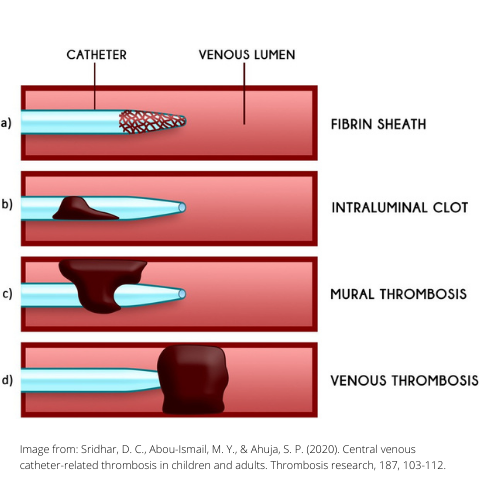
The pooled incidence of CRT, both symptomatic and asymptomatic, is estimated to range between 2.2-58%. Further research is warranted to more accurately describe the true incidence of CRT and promote better understanding around risk management.
Patency Driven by People, Processes, and Products
Korycka states that patency is driven by a combination of people, processes, and products:

Nursing staff must be trained properly in use of ultrasounds, observing correct catheter vein ratios (CVRs), and choosing and advocating for the correct number of lumens. Additionally, protocol consistency and communication are key to improving patency and overall patient outcomes. An important process in the care and maintenance of catheters is flushing. While pulsatile flushing and continuous flushing are both used to reduce catheter bacterial colonization, the 2021 INS Standards recommend using the pulsatile technique as it has been shown to be more effective at removing solid deposits. However, Korycka emphasizes that more clinical studies are needed to provide further clarity on the true effect of this technique.

Patency Products: HydroMID and HydroPICC
Polyurethane, the material used for most catheters (including CVADs, PICCs, and midline catheters) is problematic in that it invites platelet attachment. The combination of an oily and textured surface creates the perfect attachment point for platelets as they identify polyurethane as a foreign body within the blood vessel. This response is triggered immediately following catheter insertion. First, a film of plasma proteins forms on the catheter surface. These proteins then attract platelets and fibrin to the site, leading to thrombus formation and catheter occlusions.
However, new technology has shown remarkable promise in reducing risk of thrombotic complications. HydroMID® and HydroPICC® are composed of hydrophilic material that absorbs water and camouflages itself to the body’s foreign object response. In simulated environment testing, there was an average of 97% reduction in thrombus observed compared to polyurethane cathethers. An animal study revealed fully patent catheters at both days 14 and 28 of indwell duration. Additionally, a retroactive clinical study revealed a 100% reduction in occlusion complications in patients treated with
HydroPICC®.
Eloquest Healthcare is committed to providing important, timely information to help you optimize patient outcomes during vascular access procedures and maintenance. To learn more about catheter patency, HydroMID®, and HydroPICC®, view the webinar here!








