
Michelle DeVries, MPH, CIC, VA-BC, recently gave a webinar titled “Putting the Standards into Practice… and Not Stopping There!” With more than 25 years of experience, Michelle is an expert in the field of infection prevention with a focus on vascular access. Here, we’ve summarized some of the main points of her presentation. View the full webinar Here.
Vascular Access: Current Problems Create Opportunities for Progress
Examining current practices, problems, and trends in vascular access can help identify areas for future improvement. Developing a broad understanding of these issues can turn them into focal points for progress.
The COVID-19 pandemic, as you know, has taken an enormous toll on many areas of healthcare. Data published from 2020 by the CDC shows a significant spike in central line-associated bloodstream infections (CLABSIs) across hospital locations nationwide as the pandemic raged on. By the fourth quarter of 2020 there had been a 47% increase in CLABSIs reported, with 65% of that increase located within intensive care units. It is clear that reducing CLABSI rates must be a priority when updating standards and practices.
In 2021, peripheral vascular access harm gained attention as another significant problem in patient quality of care. In fact, peripheral vascular access harm was listed among the top ten patient safety concerns. Now is the best time for vascular access teams to evaluate these negative previous outcomes and make focused changes, starting today. The 2021 Infusion Therapy Standards of Practice (2021 Standards) refers to vascular access teams as clinicians “charged with the goal of accuracy, efficiency, and consistency for the delivery of infusion and vascular access services.”1 The 2021 Standards also note that although the team may not be directly involved with all vascular access prevalence rounds, they are consistently and actively involved in providing advanced knowledge to primary care staff and promoting safe practices within their facilities.1

How the Standards Are Organized: Breaking It Down
The 2021 Standards are a useful, comprehensive tool that serves to inform and support clinicians’ decisions. Michelle suggests reading the front matter first, in order to orient and familiarize yourself with the 2021 Standards overall.
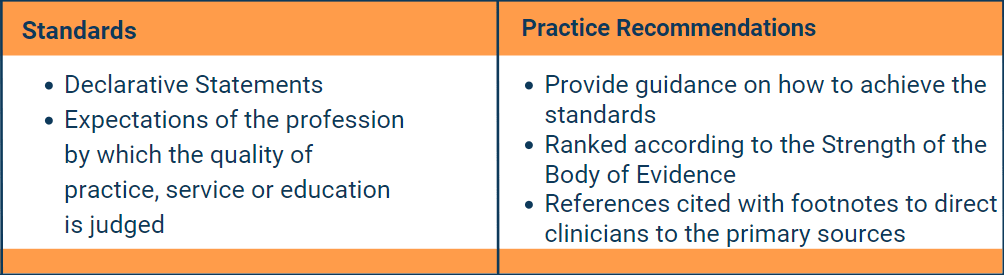
Understanding where the statements come from, how they are evaluated, and how to implement them can help you better advocate for the best care for your patient. It is important to note that there are different levels and types of evidence reported for each standard and practice.
Historically, the INS Standards have been updated every 5 years. Each version is thoroughly evaluated and reviewed before publication. In the process of creating these works, 2,500 pieces of literature were reviewed between 2015 and 2020.
The 2021 Standards
The 2021 Standards is a robust document that provides expectations and guidance on how to achieve each standard. In the webinar, Michelle focused on the following:
- Quality Improvement (Standard 6)
- Vascular Access Device Planning (Standard 26)
- Short Peripheral Intravenous Catheters
- Long Peripheral Intravenous Catheters
- Midline Catheters
- CVADs
- Vascular Access Device Removal (Standard 45)
- Vascular Access Device Assessment, Care, and Dressing Changes (Standard 42)
- Catheter Associated Skin Injury (Standard 55)
- Product Evaluation, Integrity, and Defect Reporting (Standard 12)
- Infection (Standard 50)

Using Data to Drive Continued Improvements
Vascular access is a rapidly evolving field with ongoing clinical research and data collection. There is the opportunity to influence the next edition of the Standards with work being conducted in programs today.
Michelle highlights a Quality Improvement project completed in her facility through the context of the 2021 Standards. A multi-disciplinary team aimed to increase vascular access dressing integrity rates. This team included vascular access, infection prevention, and nursing education/clinical nurse specialists with input from wound nurses and materials management representatives. The goal was to achieve 80% of dressings remaining fully intact (without reinforcement) until the device was removed or the dressing was changed at 7 days.2
When only additional staff education was used, their goal was not met. However, adding gum mastic adhesive to dressing care routines resulted in the vascular access team exceeding their goal of achieving 80% of dressings intact.2 Post implementation, the team was able to sustain results of greater than 98% fully intact dressings. Read more about their clinical outcomes Here
Michelle stresses that all levels of evidence are valuable. In order to advance practice, the time to start is now, making sure that each team’s experiences are shared throughout the facility.
Eloquest Healthcare, Inc. can partner with your institution to facilitate a Vascular Access Device Site Assessment to determine the state of both dressing and skin integrity for patients in your facility, while providing you and your team with information on your facility’s infection risk, nurse efficiency, and product waste.
Click HERE to request a Point Prevalence Assessment today!








