
Left Ventricular Assist Device (LVAD) Associated Complications
LVADs are the standard of care for patients with advanced heart failure. LVAD placement is a relatively common procedure, with more than 2,000 LVAD implants recorded each year over the past ten years in the United States alone.1
Complications that LVAD patients may experience during treatment include severe bleeding and infection. In fact, one in six LVAD patients develop a device-related infection within one year of implantation. 1
Driveline (DL) infections are the most frequently reported LVAD-related infections. The factors responsible for DL infection prevalence are: 1
- Artificial DL material, which facilitates biofilm formation
- DL exit site (often in abdominal wall) allows pathogens to enter the body
Exit Site Care Varies Between Facilities
Patients and caregivers are often responsible for exit site care at home after LVAD implantation. They must perform routine, sterile dressing changes when exit site dressings are compromised. 1

However, due to the lack of national guidelines for DL exit site dressing changes, each facility implements their own protocols. This means that there are no standardized aftercare instructions for patients and caregivers, with frequency of driveline dressing changes varying across centers. 2 This variability can also be seen in DL infection frequencies. In a review of 1,062 LVAD patients, the median reported DL infection frequency ranged between 0-52%. 1
New Evidence Supports Practices to Improve DL Dressing Durability
A study conducted by Abigail Vowels, RN, BSN recently examined whether applying standard vascular access device dressing practices to DL exit site care could:1,3
- Increase dressing durability to 7 days
- Reduce infection risk
- Promote better quality of life for patients (by decreasing time spent changing dressings and supporting an active lifestyle)
The study included 20 patients, 80% male, aged 44-82 years, with an average of 2.9 years with a LVAD (range 1-8 years with LVAD).1
Study Methods1

Patients in both control and treatment groups checked in every week for a total of 14 weeks by sending photographs of current dressings, exit sites, and new dressings. Any complications were reported as well.1
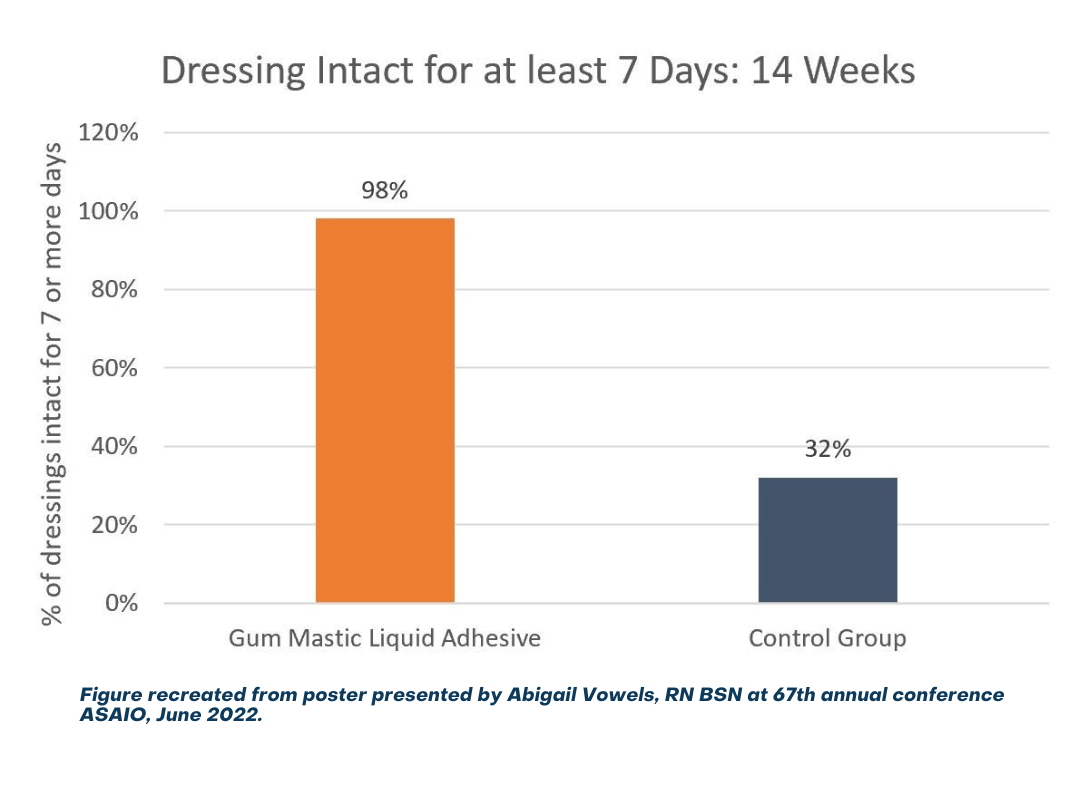
Adding gum mastic liquid adhesive and liquid adhesive remover along with patient/caregiver training significantly improved dressing integrity and durability. This can lead to the potential for fewer DL infections, improved patient quality of life, and reduced costs.1
Watch a patient describe their experience here:
View the full study here

Eloquest Healthcare is committed to providing solutions that can help improve dressing integrity and durability while reducing unnecessary costs. For more information about Mastisol or Detachol, please call 1‐877‐433‐7626 or complete this form.
Eloquest Healthcare, Inc. can partner with your institution to facilitate a Vascular Access Device Site Assessment to determine the state of vascular access device & dressing securement for patients in your facility, while providing you and your team with information on your facility’s infection risk, nurse efficiency, and potential product waste. Click here to request a Vascular Access Device Site Assessment today!

References:
- Vowels A. Impact of Using Gum Mastic Liquid Adhesive on Integrity and Durability of Driveline Dressings to Reduce Risk of Infection and Improve Quality of Life. Poster presentation at 67th Annual Conference ASAIO. Chicago, IL: June 8-11, 2022.
- International Consortium of Circulatory Assist Clinicians. ICCAC Best Practice Consensus Guidelines: Driveline Management. 2020.
- Guidelines for the Prevention of Intravascular Catheter-Related Infections, 2011.







