
Of the 200 million people worldwide who have been diagnosed with diabetes, millions receive their diabetes care through insulin pump therapy and use continuous glucose monitors (CGMs) and insulin pumps.[1] This may result in improved diabetes care and greater control over users’ blood glucose levels.
“My overall health is better. Insulin delivery is better, so treatment is more consistent. With the continuous glucose monitor, I like to know what my levels are sooner—that information is more accessible. At first I was resistant, but now I like it and miss it when I’m not wearing it”[2 ]– Al, diabetic patient, CGM wearer, and insulin pump user
Patients who use continuous glucose monitoring have reported the benefit of being able to see and predict their blood glucose level trends, allowing for more refined diabetes management.[2] However, continuous glucose monitor users may also experience a wide array of other concerns, including social stigma, problems while traveling, difficulty with applications, trouble leading an active lifestyle, and the risk of serious infection.[3,4]

“I don’t like the CGM in my abdomen, and my arm is a place that I don’t do insulin injections, so it’s not beat up. It’s hard to get in there, though, and my wife actually puts it on for me.” – Al, diabetic patient, CGM wearer, and insulin pump user
Moving Injection Sites
For effective diabetes management, it is recommended that insulin pump users change their infusion site every two to three days,[5] and sometimes, assistance may be necessary in changing the infusion site.[2] With experience, however, many patients can get used to their insulin pump supplies and become adept and efficient at changing infusion sites.
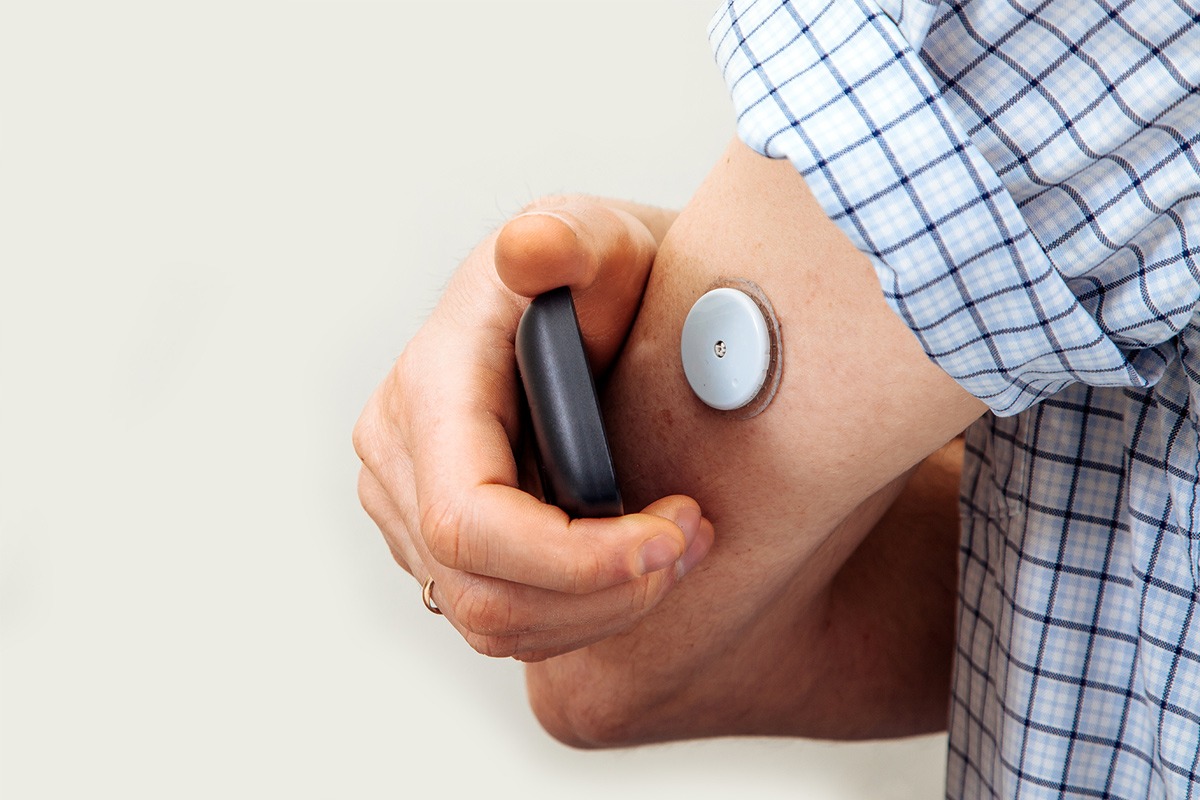
“If you put me on a clock, I can change the pump in 3 minutes”. – Al, diabetic patient, CGM wearer, and insulin pump user
While changing sites is best practice and essential for keeping tissue healthy, promoting absorption, and avoiding hypertrophy, doing so can also cause other complications to arise.[5]
Insulin Pumps and Infection
Moving the infusion site may also be required if a pump becomes loose because the skin becomes sweaty after exercising.6 When attaching a pump to a new infusion site, to avoid infection and promote adherence, it is recommended that those on insulin pump therapy clean and dry each infusion site. However, repeated sensor securement and sensor removal can cause the skin to become agitated, and irritated skin may increase the likelihood of infection.[5]
These infusion site infections can range from abscesses and cellulitis.[7] While Staphylococcus aurerus is the most common cause, other organisms can cause more serious problems, including bloodstream infections.[7] Whenever the dermal layer is punctured, there is an increased risk of infection, and an increased number of punctures causes even more opportunity for an infection to take hold. A firm seal between the insulin pump and the skin can cause fewer unintended infusion site relocations, helping to promote sterility at injection sites.[4]
Minimizing infection risk is an essential part of optimizing “The Triple Aim” of the Affordable Care Act. Eloquest Healthcare is committed to providing solutions that can
help you reduce the risk of conditions like a central line-associated bloodstream infection (CLABSI) and post-operative wound contamination.

References:
1. American Diabetes Association. Insulin Pumps Need Greater Safety Review: American Diabetes Association Issues Joint Statement with European
Association for the Study of Diabetes. Retrieved from http://www.diabetes.org/newsroom/press-releases/2015/insulin-pumps.html.
2. Al T., personal communication, November 8, 2018.
3. Liu NF, Brown AS, Younge MF, Guxman SJ, Close KL, Wood R. Stigma in people with type 1 or type 2 diabetes. Clin Diabetes. 2017;35(4):262-262.
4. Information About Diabetes. Preventing and Treating Insulin Pump Site Infections. Retrieved from http://www.informationaboutdiabetes.com/lifestyle/lifestyle/preventing-and-treating-insulin-pump-site-infections.
5. Insulin Pumpers: Support and Information for Adults and Children with Diabetes. Tape Tips and Other Infusion Site Information. Retrieved from http://www.insulin-pumpers.org/howto/tapetips.shtml.
6. Diabetes Net. Sweating. Retrieved from https://www.diabetesnet.com/diabetes-technology/insulin-pumps/pump-life/pump-problems/sweating.
7. Diabetes Health. Got Pump Bumps? Retrieved fromhttps://www.diabeteshealth.com/got-pump-bumps/.







