
The US Centers for Disease Control and Prevention (CDC) and The Infusion Nurses Society (INS) agree that vascular access device (VAD) dressing integrity is a critical factor for the prevention of hospital-acquired infection.1,2
Russell Nassof, JD, founder of RiskNomics, discusses the importance of common sense in evidenced-based medicine, the issue of dressing disruption, the prominence of Medical Adhesive-Related Skin Injury, small evidence-based studies, and the potential legal and financial implications of dressing disruption in a 50-minute educational webinar available here. In this blog, we’ll provide the highlights of his presentation.
Evidence-Based Medicine
When treating patients, physicians need to not blindly rely upon Clinical Practice Guidelines, but rather use common sense and make changes when changes are needed. Evidence-based medicine relies upon clinical judgement and critical thinking, current scientific evidence and patient values and preferences to provide a high level of care.3,4
Dressing Disruption and Risk of Infection
Both the CDC and Infusion Therapy Standards of Practice recommend that catheters be replaced if the insertion or dressing becomes damp, loosened, or visibly soiled.1,2 In fact, dressing disruption is a major risk factor for catheter-related infections.5
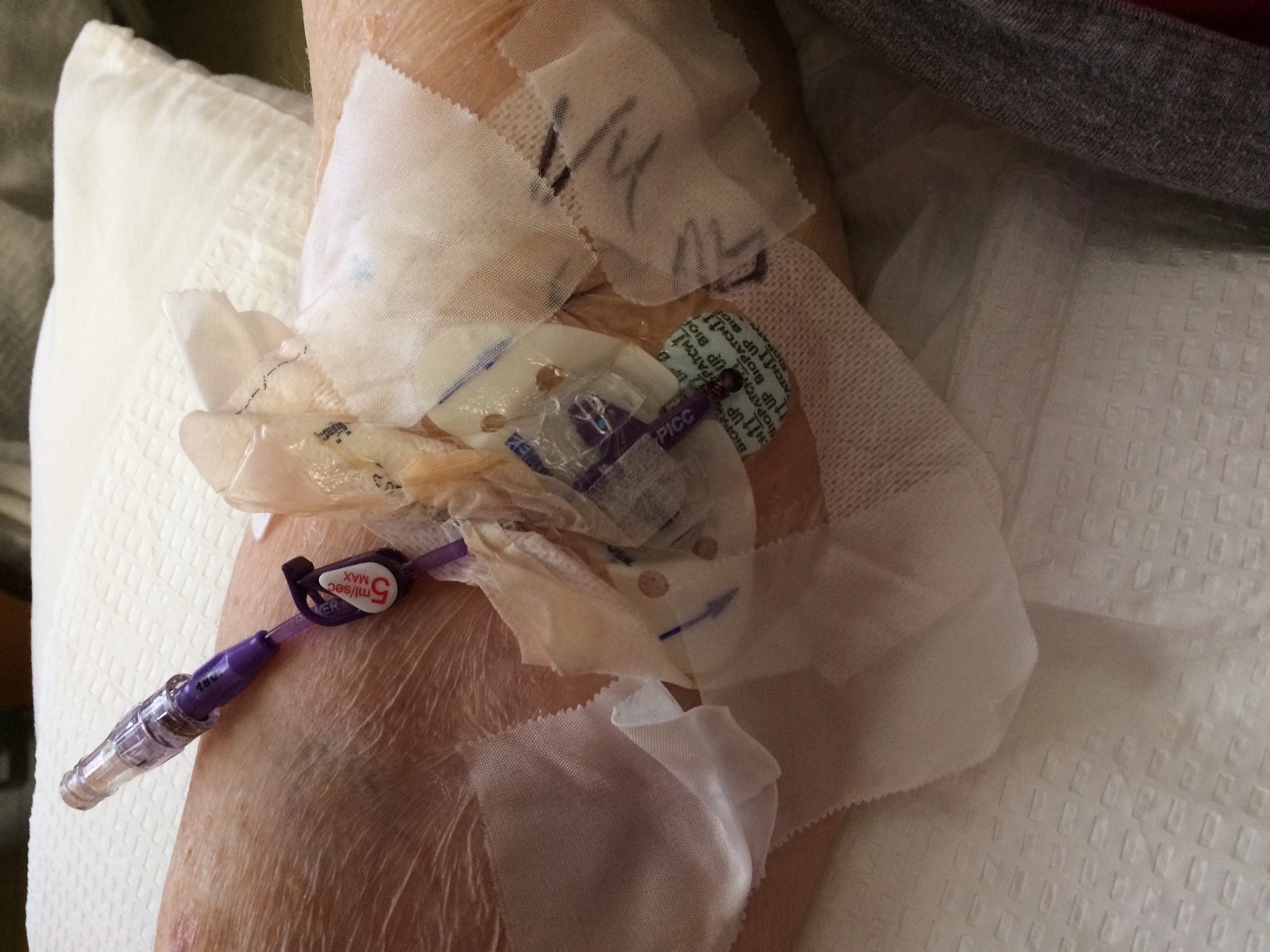
One study demonstrated that only 3% of dressings lasted the entirety of their intended 7 days with a majority of dressings lasting less than 48 hours,6 and another study found that 67% of over 11,000 dressing changes were performed earlier than scheduled due to soiling or becoming non-adherent.5
MARSI
MARSI, or Medical Adhesive-Related Skin Injury, is a persistent issue in the medical space. MARSI is defined as an occurrence in which erythema or another manifestation of cutaneous abnormality persists for 30 minutes or more after the removal of a medical adhesive product.7 However, it should be noted that improved dressing integrity results in a decreased need for dressing changes and therefore a reduced risk of MARSI.8 Additionally, healthcare providers should consider the use medical adhesive removers to minimize skin discomfort and skin damage associated with removal of adhesive products.7
The Legal Argument
Today, more and more medical complications are deemed preventable, and the risk of a malpractice claim is higher. Healthcare providers must now ask themselves if a hospital-acquired infection (HAI) was at all preventable and if the standard of care was met.
What’s more, providers must also consider any products available to address the issues at hand and if using those products would have resulted in improved patient outcomes with minimal risk, liability, cost, and training.
As a whole, INS, CDC, and National Evidence-based Guidelines for preventing HAIs must be considered. The evidence from 4 small studies is :




Finances and Dressing Disruption
Cost reduction is associated with minimized dressing changes, each of which costs anywhere from $5 to $9.50.5 There is also a time-saving element due to fewer dressing changes,6 as well as the psychological savings that come from improved patient comfort.14
Incorporating clinical practice guidelines with evidence-based medicine is the best way to ensure that we are meeting the standard of care. Numerous studies have clearly indicated that the prevention of dressing disruption is pivotal in reducing the risk of infection. Using a product that enhances the potential for catheter dressings to remain adherent may assist clinicians in meeting evidence-based standards of care and decreasing the prevalence of CRBSIs, all while reducing costs and improving both patient and clinician satisfaction.
Minimizing infection risk is an essential part of optimizing “The Triple Aim” of the Affordable Care Act. Eloquest Healthcare is committed to providing solutions that can help you reduce the risk of conditions like a central line-associated bloodstream infection (CLABSI) and post-operative wound contamination.

References
- O’Grady NP, Alexander M, Burns LA, et al. Guidelines for the prevention of intravascular catheter-related infections, 2011. https:// www.cdc.gov/hicpac/pdf/guidelines/bsiguidelines 2011.pdf. Accessed January 8, 2019.
- Vascular Access Device Management. In: Infusion Therapy Standards of Practice. J Infus Nurs.2016; S68- 94.
- Monico E, Moore C, Calise A. The Impact of evidence-based medicine and evolving technology on the standard of care in emergency medicine. Internet Journal of Law, Healthcare and Ethics. 2004;3:1-7.
- Sackett, DL, Rosenberg WMC, Gray JAM et al. Evidence-based Medicine: what is is and what it isn’t.
- Timsit JF, Bouadma L, Ruckly S, et al. Dressing disruption is a major risk factor for catheter-related infections. Crit Care Med. 2012;40:1707-14.
- Richardson A, Melling A, Straughan C. Central venous catheter dressing durability: an evaluation. J Infect Prev. 2015;16:256-61.
- McNichol K, et al. Medical Adhesives and Patient Safety: State of the Science, J Wound Ostomy Continence Nurs. 2013;40(4):365-80.
- Ryder M, Duley C. Evaluation of compatability of a gum mastic liquid adhesive and liquid adhesive remover with an alcoholic chlorhexidine gluconate skin preparation. J Infus Nurs. 2017;40(4)245-52.
- Browne B, Moffo H. Quality Improvement Initiative Results in Fewer Dressing Disruptions and Improved Adherence to Best Practices. Presented at: Greater Cincinnati AACN Chapter, 28th Annual Trends in Critical Care Conference, April 8, 2016.
- Devries M, Sarbenoff J, Wickert M. Addressing the dressing: Improving dressing disruption in vascular access. Presented at Canadian Vascular Access Association Conference, April 25-27, 2018. Toronto, Ontario, Canada.
- Bortz A, Hardinger K, Peltzer J. Impact of implementing Mastisol in central line dressing changes on central line-associated blood stream infections in progressive care units: a quality improvement project. Presented at: Magnetizing KC Symposium, February 24, 2015. Kansas City, KS.
- Pullen, D. Quality improvement initiative to improve dressing adherence reveals improved dressing adherence observations on a before-after analysis. Presented at AVA Annual Scientific Meeting, September 7-10, 2014. Washington, D.C.
- Scott, R. The direct medical costs of healthcare-associated infections in US hospitals and the benefits of prevention. 2009. https://www.cdc.gov/HAI/pdfs/hai/Scott_CostPaper.pdf Accessed January 10, 2019.







